Hundreds of millions of people suffer from depression worldwide, and up to 44% of these people have not found relief from typical antidepressant therapies. This ‘treatment-resistant’ form of depression is especially devastating, as patients can suffer for many years without hope of recovery.
Even patients who find some form of relief from the usual prescribed antidepressants need frequent doses, causing unpleasant side-effects, and these drugs often lose their effectiveness after several years of treatment. What we really need, argue many psychiatrists and mental health professionals, is a paradigm shift in the way we treat depression. It’s looking very likely that psychedelics could trigger this change.
THE DEFAULT MODE NETWORK
Much of the recent research into depression has focused on the Default Mode Network (DMN). This is a system in the brain that is a core aspect of our consciousness and sense of self. When you are remembering the past, daydreaming, or thinking about yourself or others, the DMN is active. The DMN is found to be overactive in patients with major depression, perhaps causing an increase in the intensity of negative thoughts.
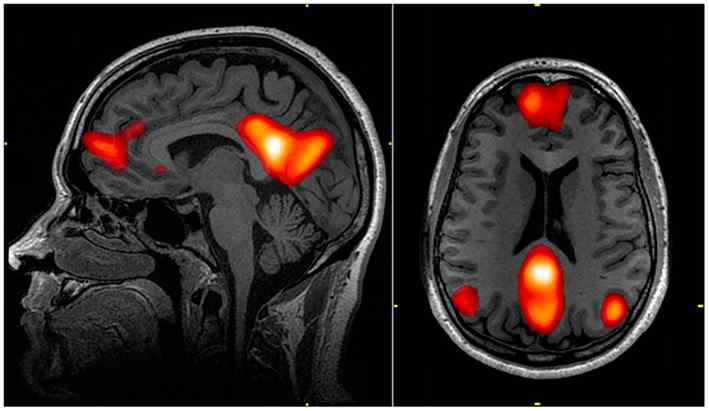
The Default Mode Network (DMN) as it appears in MRI scans. The DMN is a complex system that keeps our consciousness in check, and is overactive in depression. Adapted from Graner et al. (2013)
Some promising research has shown that psychedelics may possess antidepressant properties, through their interaction with the DMN. Several pilot studies from the group of Professor David Nutt in London have led the charge. One of these studies used psilocybin-assisted therapy to treat 12 people suffering from treatment-resistant depression, and other studies investigated the potential antidepressant effects that psychedelics might have in the brain.
PILOT STUDY OF PSILOCYBIN TREATMENT FOR DEPRESSION
The psilocybin study, led by Dr. Robin Carhart-Harris, specifically set out to treat sufferers of depression with psychedelic therapy. Twelve patients with severe depression, who had failed to find relief from typical treatments of depression, were given two doses of psilocybin, seven days apart, in a comfortable environment. A clinical psychologist was present for both sessions to provide support and guidance. The first session was a moderate dose of psilocybin (10mg) and the second session was a high dose of psilocybin (25mg).
The patient’s depressive symptoms were measured before, one week after, and three months after the trial using an approved scoring system. All the patients showed improved depression scores after a week, and seven patients retained this improvement after three months.
Impressively, five of the patients went from a score of ‘severe depression’ to a score of ‘no depression’ immediately following the psilocybin therapy. After three months, five of the patients (who started with either severe or moderate depression) were scored as having no depression.
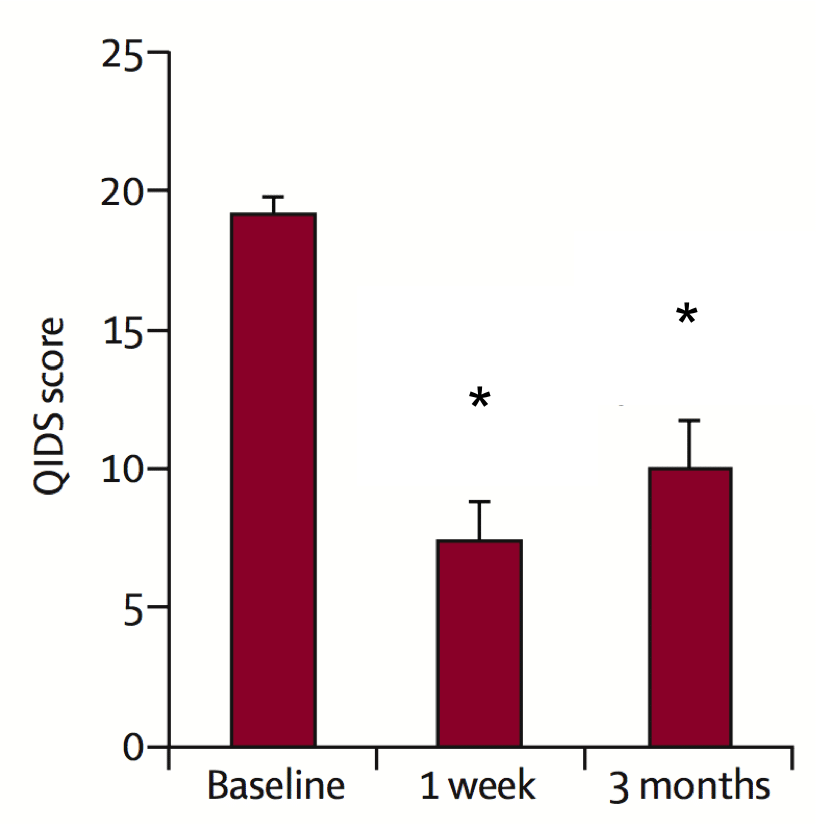
Psilocybin caused a significant decrease in depression scores in 12 patients lasting at least three months. Adapted from Carhart-Harris et al. (2016)
Although this was a small study, it remains a promising step forward into establishing psilocybin as a potential treatment for depression, when used as a therapeutic tool in the correct setting. The fact that this treatment could effectively reduce depression scores (sometimes to zero!) and keep depression at bay for at least three months in most patients, is really encouraging. Compared to typical antidepressant therapy programs, these early results look very impressive.
How could psilocybin have such a dramatic effect on people’s depression?
PSYCHEDELICS AND THE DEFAULT MODE NETWORK
An earlier study by Dr. Carhart-Harris looked at the changes within the brain caused by psilocybin, in ordinary non-depressed people. The researchers found that psilocybin disrupts the DMN, a part of the brain that ties together our normal consciousness. By disrupting the DMN, psilocybin releases consciousness from its stringent control mechanisms. By allowing consciousness to break free of this control, psychedelics enable depressed people to move outside of their recurrent negative thoughts.
Others from Professor Nutt’s group in London wanted to expand on these results and performed the first ever brain imaging study using LSD.
By disrupting the DMN, psychedelics release consciousness from its stringent control mechanisms.
Prof Nutt’s group took extensive images of people’s brain activity after they’d been given a moderate dose of LSD (75ug). The results are complex, but one of the most interesting findings concerned the DMN; Nutt’s group discovered that LSD reduced the activity of the DMN, in a similar way to psilocybin. The researchers found that, the more the DMN was disrupted by LSD, the more their participants experienced ‘ego dissolution’, meaning patients lost their sense of self and became less focused on the typical worries of everyday life.
Although these are early studies – and we don’t know anything for certain yet – it looks like two classic psychedelics – LSD and psilocybin – could catalyze a paradigm shift in psychiatry.
We’ve been treating depression as a simple chemical imbalance that we can treat with frequent pharmacological intervention, but it has not worked as planned. Depression is a disorder in the complex, high-level parts of consciousness such as the DMN. We need a treatment that changes the way people think. Psychedelics, by disrupting the DMN and opening up consciousness to new ways of thinking, could be that treatment.
If you want to find out more about the topic check out our podcast interview with Dr. Julie Holland, M.D. talking about Connection Through Chemistry or Click here to read the transcript
Grow 1 Year's Worth of Microdoses in Just 6 Weeks
Third Wave partnered with top mycologists to create the world’s easiest and best mushroom growing program (kit, course, and expert support).
- Pre-sterilized and sealed
(ready to use out of the box) - Step-by-step video and text course
- Access to growing expert in community
- Make your first harvest in 4-6 weeks
- Average yield is 1 - 4 ounces (28-108g)
- Fits in a drawer or closet
- Enter info for Third Wave discounts:


Grow 1 Year's Worth of Microdoses in Just 6 Weeks
Third Wave partnered with top mycologists to create the world’s easiest and best mushroom growing program (kit, course, and expert support).
- Pre-sterilized and sealed
(ready to use out of the box) - Step-by-step video and text course
- Access to experts in community
- Make your first harvest in 4-6 weeks
- Average yield is 1 - 4 ounces (28-108g)
- Fits in a drawer or closet
- Enter info for Third Wave discounts
RECENT FINDINGS WITH AYAHUASCA
The most recent comprehensive study on psychedelics as a treatment for depression focusses on the ancient psychedelic brew ayahuasca. There have been anecdotal reports of ayahuasca experiences curing people of their depression, with the psychedelic trance being described as being like hundreds of therapy sessions condensed into a matter of hours.
This study is now the first to offer a randomised, placebo-controlled clinical study of the anti depressive effects of the ayahuasca experience. 29 patients with severe depression were given either one session of ayahuasca or a placebo, then analysed for changes in their depression scores. One day immediately following the sessions, the ayahuasca group scored significantly lower on depression tests compared to the placebo group. After seven days, the placebo group had returned to a normal depression level, while the ayahuasca group were still on a much lower depression score.
It’s important to emphasise that this study was conducted in a therapeutic, supportive environment. If ayahuasca does indeed possess antidepressant effects, it almost certainly needs to be consumed in a prepared, responsible and therapeutic environment.
THE BIPARTITE MODEL OF DEPRESSION
The mounting evidence of psychedelics’ effectiveness at treating depression has led some scientists to develop a new theory of depression. Know as the ‘bipartite’ model, it suggests that while antidepressants work through serotonin 1A receptors (known as a ‘coping’ mechanism), psychedelics work through serotonin 2A receptors (known as an ‘adaptive’ mechanism). This theory explains how antidepressants are effective at treating symptoms in many people – yet, why psychedelics could be required to produce lasting changes in perception and mood. Read more about this model here.
HOW CAN THIS HELP YOU?
If you or a loved one suffers from depression, psychedelics could help you. However, it’s important to note that in these studies, sufferers of depression were given extensive psychotherapy and took their psychedelics in a comfortable, controlled environment.
Taking a huge dose of LSD at home alone is unlikely to be as therapeutic. If you decide to use macrodoses of psychedelics to self-treat depression (which we don’t recommend as we’re not healthcare professionals), try to minimize risks by following the six S’s of psychedelic use. Alternatively, many individuals have treated their depression with a microdose, instead of a high dose. You can see some reports from individuals who have used microdosing in this way here.
If you want to learn how to microdose with expert guidance rather than going it alone, sign up for our Microdosing Course. Using the latest research from cutting-edge scientists and doctors, we’ll help you develop a customized, step-by-step process to change habits, enhance creativity, and optimize performance.
Curious about supporting your mental health through psychedelics? Check out Third Wave’s vetted directory of psychedelic therapists.
Important Note: This is a constantly evolving document. If you believe we’re missing something important, please let us know via the contact page.









I have suffered from depression for most of my adult life. At times it’s been a very deep dark ordeal lasting years. Conventional medications seem to have no effect. The only way I’ve noticed they do anything at all, is when I stop doing them, and my condition worsens. I hadn’t tried psychedelic substances because I was afraid it would accentuate the problem. When I finally found the courage to try mushrooms, I was pleasantly surprised that depressive symptoms subsided for at least a couple weeks. My friends pointed out that the tremors I have had for years, (perhaps from the psych meds) subsided immediately upon using the mushrooms. In the last couple years I’ve increased the dosage, and have noticed the period of relief has increased to 2 or 3 months. I am still on the psych meds as when I tried to eliminate them I crashed hard. I am functioning very well with a fairly high dose of cubensis ( 3.5 grams) every 3 months. I prefer to do them alone in a comfortable environment. This has been the best I’ve felt in my entire adult life. I wish there were more research done with psyliciben. Somewhere there may be a better treatment perhaps with microdosing, that could eliminate the need for the conventional psych meds.
I’ve been a recreational user of psychedelics before I got depressed (I sufferd post partum depression after my daughter was born). A year after her birth I was still feeling like crap most of the time, crying, anxious and feeling dull. I gave LSD a try again. And man I have not felt this good in that whole misrble year. I laughed during my whole trip like I had to catch up on not having a laugh for the past year. I did some more LSD trips in the months after that and I am feeling reborn. Energized, happy and I feel like great mom! Ofcourse time also played it’s part, and the fact that babies tent to sleep better after a while, but still I think LSD speeded up the process and gave me much more that I could have imageded
Thank you for sharing and spreading awareness! I hope that this magical plant would not be abused and misused. Everything, if used properly and moderately proves to be beneficial. I hope this could be the future treatment of a lot of diseases. It has endless capabilities!